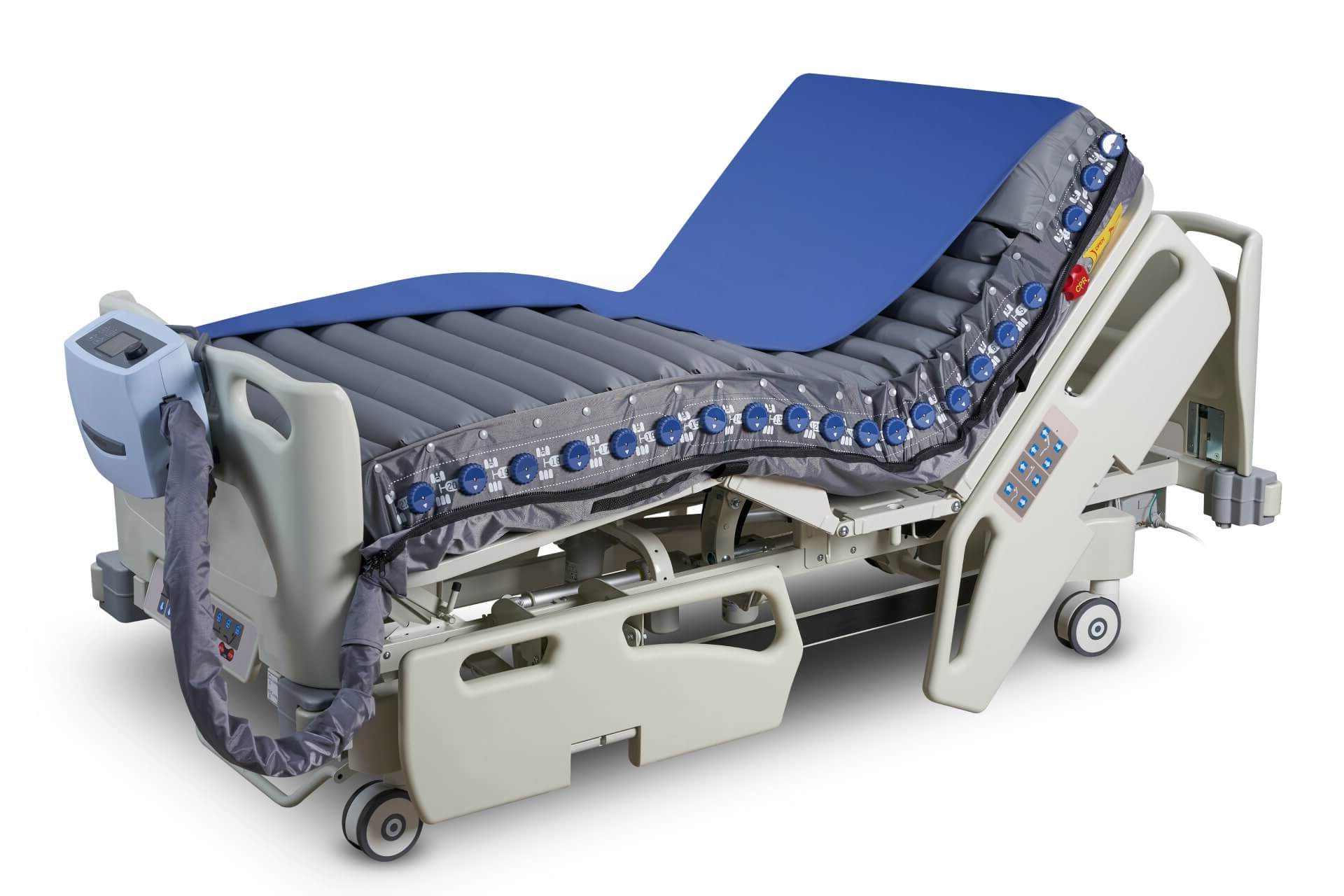
Pressure injury prevention
Pressure injuries (PIs) affect more than seven million patients worldwide each year. In the United States alone, they drive an estimated US$9—1 billion in annual healthcare spending. Manual turning and repositioning —while essential —also place sustained physical strain on caregivers, contributing to musculoskeletal injuries among nurses and care teams.
Automated air-mattress systems that support redistribution of pressure, turning, and repositioning can improve patient outcomes, protect workplace health, and help hospitals allocate staff time and resources where they matter most.
Clinical evidence
Pressure ulcers are common, costly, and global —and they may begin during surgery or immobility. In severe cases they can be life-threatening. Surfaces that redistribute pressure and support scheduled turning and repositioning can enable earlier intervention and more consistent prevention.
View clinical evidence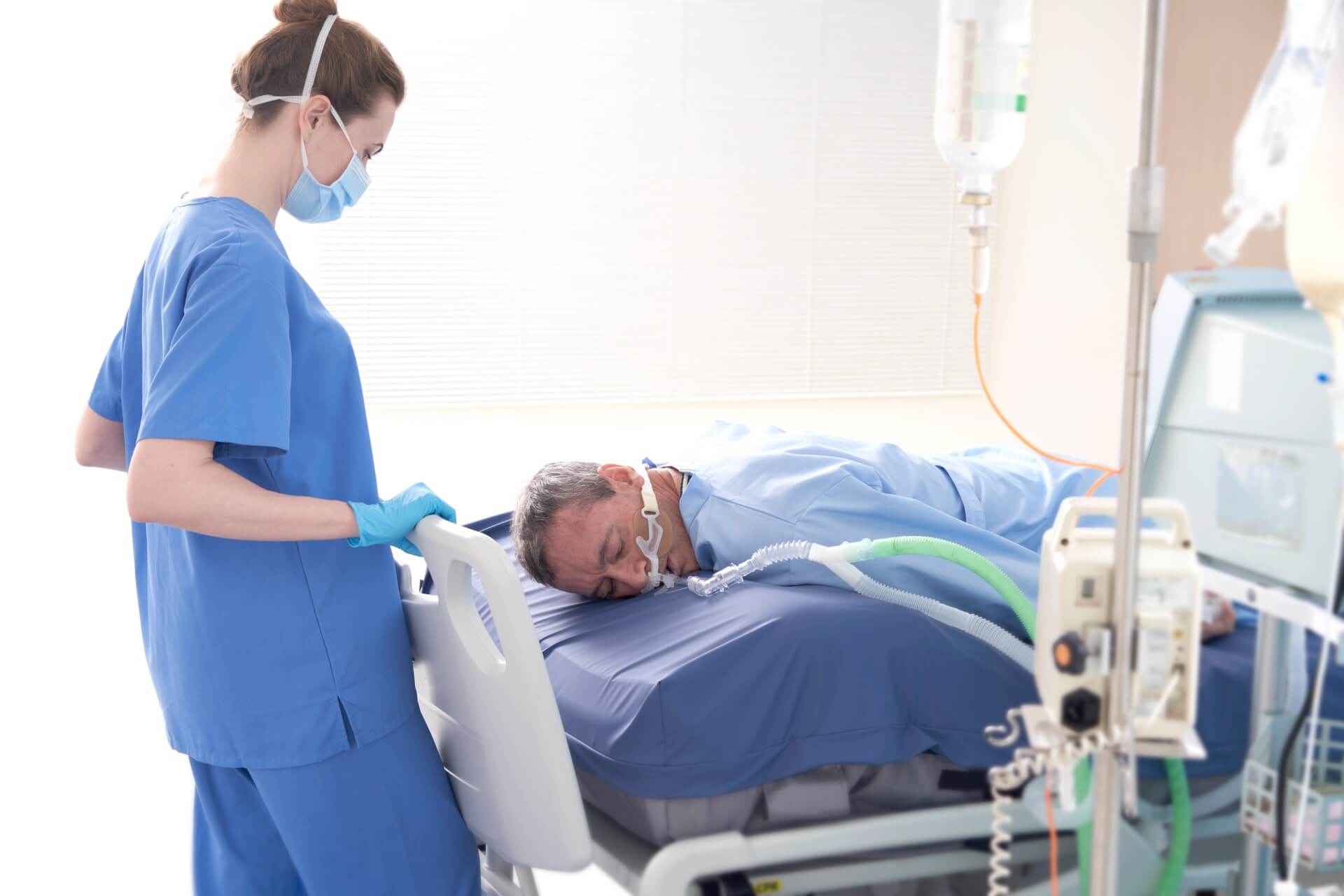
Value proposition
Managing hospital-acquired pressure injuries is expensive: treatment can reach at least US$250,000 per affected inpatient, with estimates of around US$2,122 in additional daily hospital costs. Alternating-pressure (active) support surfaces can improve comfort and help reduce pressure-ulcer incidence when used as part of a broader prevention programme.
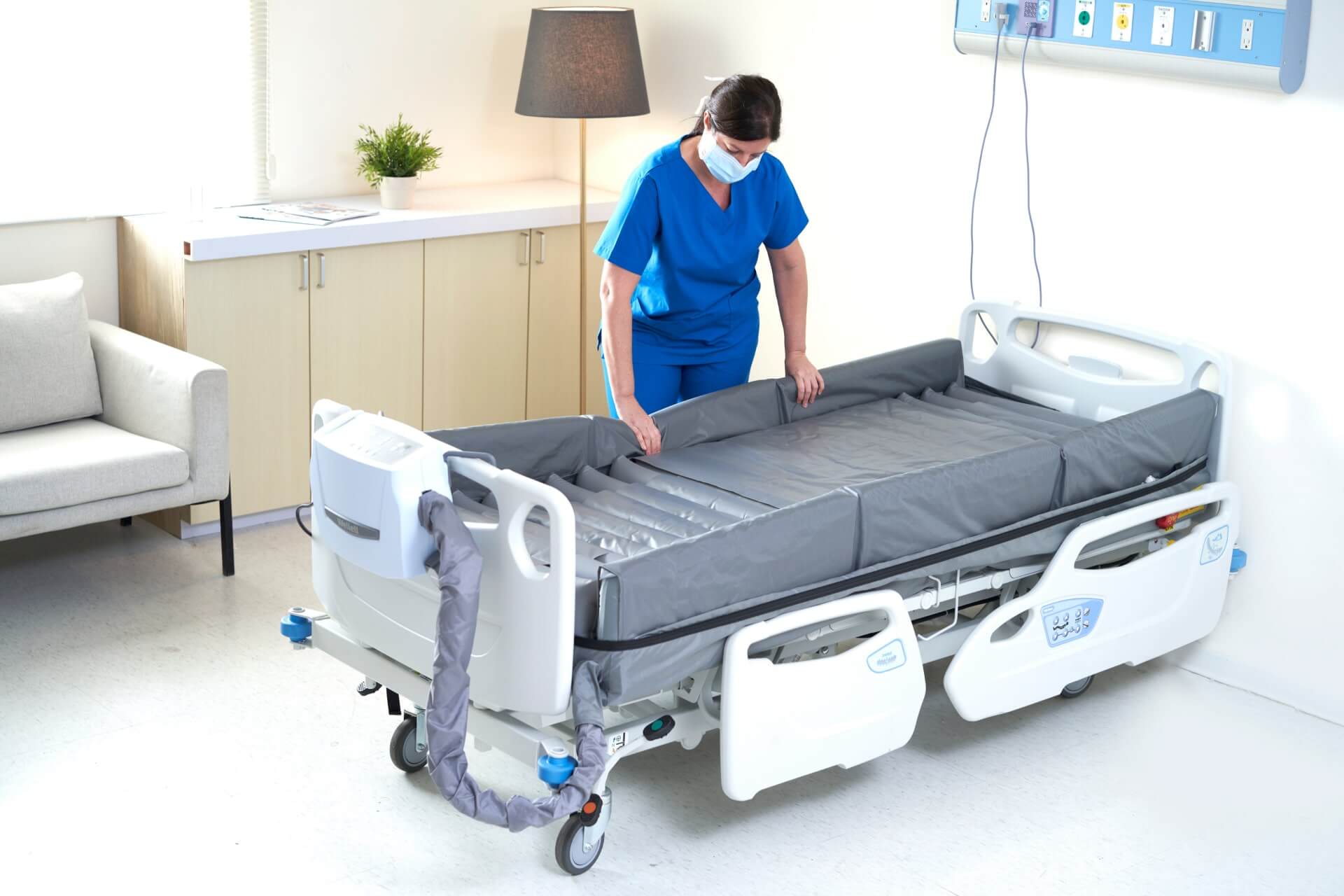
Related products

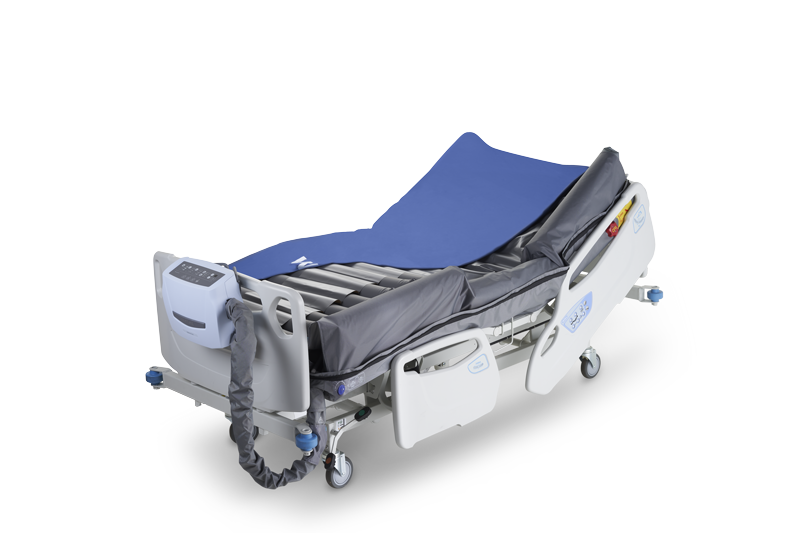
Optima Turn
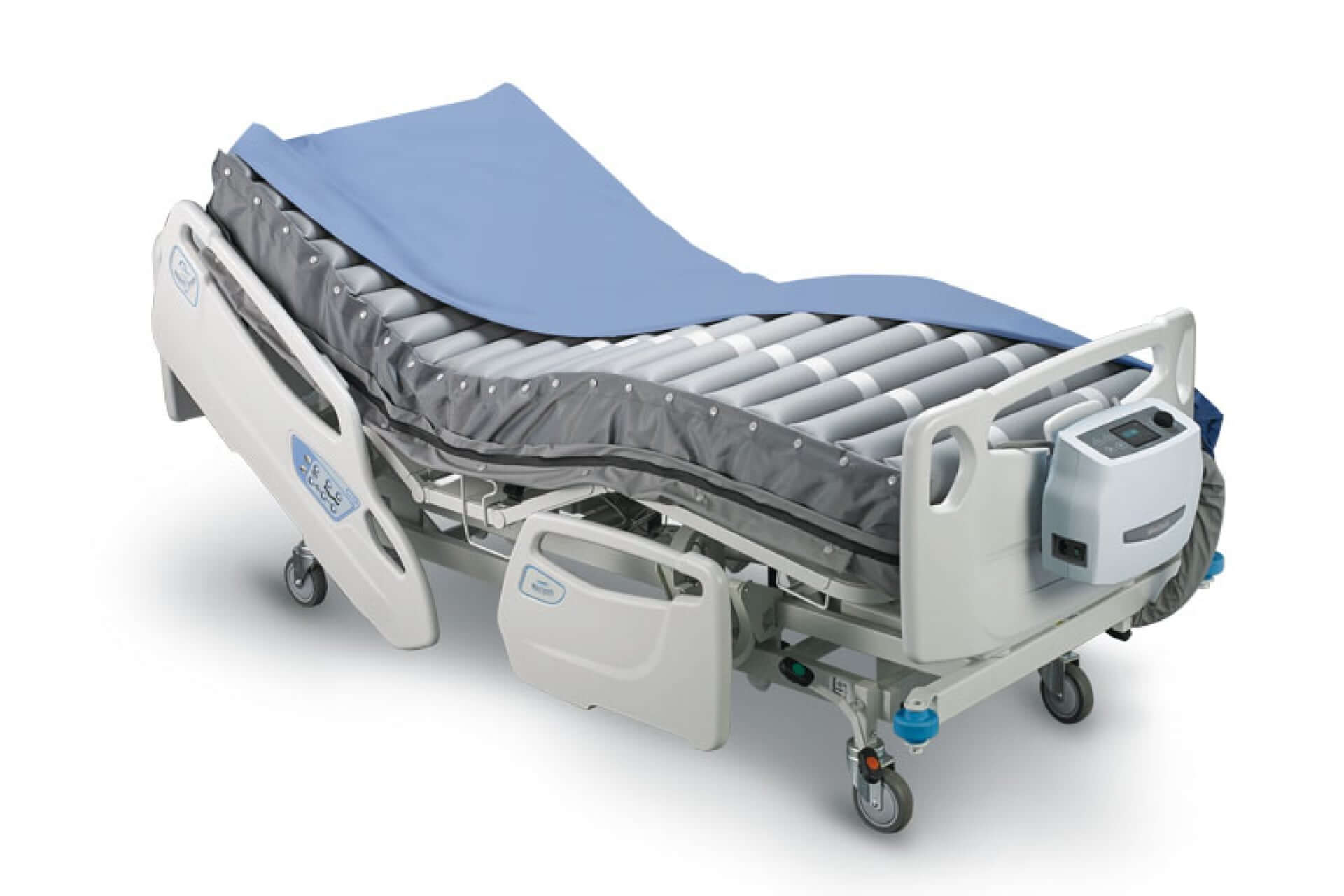
Optima Auto
References
- Padula WV, Pronovost PJ, Makic MBF, Wald HL, Moran D, Mishra MK, Meltzer DO. Value of hospital resources for effective pressure injury prevention: a cost-effectiveness analysis. BMJ Qual Saf. 2019 Feb;28(2):132-141. doi: 10.1136/bmjqs-2017-007505. Epub 2018 Aug 10. PMID: 30097490; PMCID: PMC6365919.
- Hignett S. Intervention strategies to reduce musculoskeletal injuries associated with handling patients: a systematic review. Occup Environ Med. 2003 Sep;60(9):E6. doi: 10.1136/oem.60.9.e6. PMID: 12937202; PMCID: PMC1740617.
- Dawson AP, McLennan SN, Schiller SD, Jull GA, Hodges PW, Stewart S. Interventions to prevent back pain and back injury in nurses: a systematic review. Occup Environ Med. 2007 Oct;64(10):642-50. doi: 10.1136/oem.2006.030643. Epub 2007 May 23. PMID: 17522134; PMCID: PMC2078392.
- Burke RE, Whitfield EA, Hittle D, Min SJ, Levy C, Prochazka AV, Coleman EA, Schwartz R, Ginde AA. Hospital Readmission From Post-Acute Care Facilities: Risk Factors, Timing, and Outcomes. J Am Med Dir Assoc. 2016 Mar 1;17(3):249-55. doi: 10.1016/j.jamda.2015.11.005. Epub 2015 Dec 20. PMID: 26715357; PMCID: PMC4847128.
- Vangilder C, Macfarlane GD, Meyer S. Results of nine international pressure ulcer prevalence surveys: 1989 to 2005. Ostomy Wound Manage. 2008 Feb;54(2):40-54. PMID: 18382042.
- Shafipour V, Ramezanpour E, Gorji MA, Moosazadeh M. Prevalence of postoperative pressure ulcer: A systematic review and meta-analysis. Electron Physician. 2016 Nov 25;8(11):3170-3176. doi: 10.19082/3170. PMID: 28070249; PMCID: PMC5217808.
- Black JM, Edsberg LE, Baharestani MM, Langemo D, Goldberg M, McNichol L, Cuddigan J; National Pressure Ulcer Advisory Panel. Pressure ulcers: avoidable or unavoidable? Results of the National Pressure Ulcer Advisory Panel Consensus Conference. Ostomy Wound Manage. 2011 Feb;57(2):24-37. PMID: 21350270.
- Shi C, Dumville JC, Cullum N, Rhodes S, Jammali-Blasi A, McInnes E. Alternating pressure (active) air surfaces for preventing pressure ulcers. Cochrane Database Syst Rev. 2021 May 10;5(5):CD013620. doi: 10.1002/14651858.CD013620.pub2. PMID: 33969911; PMCID: PMC8108044.